That sensation of fullness or pressure in your ears—like you’re underwater or hearing through cotton wool—is one of the most common complaints we encounter in clinical audiology practice. In our Forestville clinic, we commonly see patients who’ve been living with blocked ears for days or even weeks, uncertain whether they should wait it out or seek professional help. The frustration is understandable: your ears feel clogged, sounds seem muffled, and you might find yourself constantly trying to “pop” them for relief.
While the sensation of blocked ears is incredibly common, the underlying causes can vary significantly, from simple earwax accumulation to more urgent conditions requiring immediate medical attention. Understanding what’s happening in your ears—and knowing when to seek help—can make the difference between a simple solution and prolonged discomfort or, in rare cases, permanent hearing changes.
This article explores the most common reasons why your ears feel blocked, the diagnostic approach audiologists use to identify the cause, and clear guidance on when you should book an appointment with your GP, visit an audiologist, or seek urgent care.
Understanding That “Blocked” Feeling
Before we explore specific causes, it’s worth understanding what you’re actually experiencing. The sensation of blocked ears can manifest in several ways:
– A feeling of fullness or pressure in one or both ears
– Muffled or reduced hearing
– Your own voice sounding unusually loud in your head (autophony)
– A sensation that needs to “pop” but won’t
– Reduced clarity of sound, particularly in noisy environments
– Discomfort or awareness of your ears without actual pain
The ear is a remarkably complex system, and this blocked sensation can originate from the outer ear canal, the middle ear space behind the eardrum, or occasionally from the inner ear itself. Identifying which part of your auditory system is affected is the first step towards appropriate treatment.
Earwax: The Most Common Culprit
Cerumen—commonly known as earwax—is by far the most frequent cause of that blocked ear sensation. Your ears produce wax naturally as a protective mechanism, trapping dust, debris, and potentially harmful microorganisms before they can reach your eardrum. For most people, earwax migrates naturally outward, falling away without intervention.
However, several factors can disrupt this self-cleaning process. Regular use of earbuds or hearing aids can push wax deeper into the canal rather than allowing it to migrate out. Cotton buds, despite their ubiquity in bathroom cabinets across Australia, tend to compact wax against the eardrum rather than removing it—this is why audiologists and GPs consistently advise against their use inside the ear canal.
Some individuals simply produce more wax than others, or have narrower ear canals that are more prone to accumulation. Occupations that involve dusty environments can also accelerate wax build-up. Interestingly, many patients report that one ear feels blocked more than the other, which often reflects anatomical differences between your ear canals or variation in wax production.
When wax is the cause, you’ll typically notice gradual onset of symptoms over days or weeks. Hearing becomes progressively muffled, and you might experience that characteristic feeling of fullness. Importantly, earwax blockage alone shouldn’t cause significant pain—if you’re experiencing earache alongside the blocked sensation, another cause is more likely.
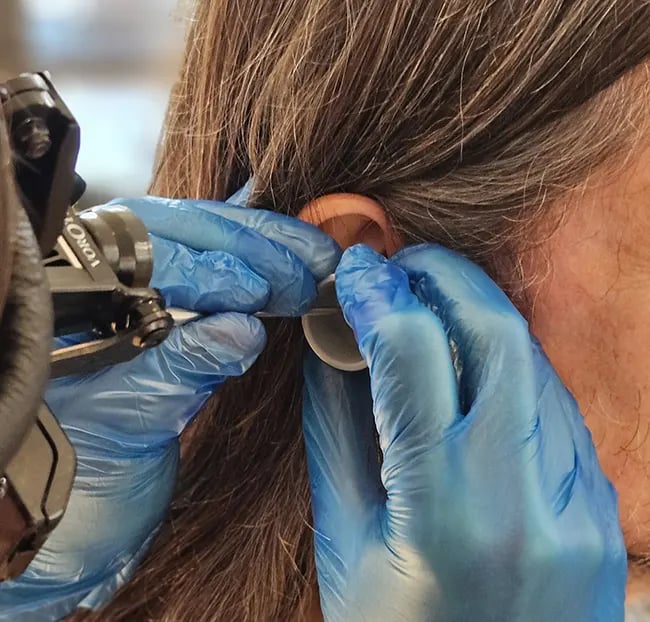
Professional ear cleaning by an audiologist or GP using microsuction, irrigation, or manual removal under direct visualisation is the safest and most effective approach. At The Audiology Place, we use video otoscopy during wax removal procedures, allowing both clinician and patient to see exactly what’s happening throughout the process.
Eustachian Tube Dysfunction: When Your Ears Won’t Pop
The Eustachian tube is a narrow passage connecting your middle ear to the back of your nose and throat. This tube serves a crucial function: equalising air pressure on both sides of your eardrum. When functioning properly, you barely notice it—perhaps only during altitude changes on flights or when driving through mountainous terrain.
Eustachian tube dysfunction (ETD) occurs when this tube doesn’t open and close properly, creating pressure imbalance and that persistent blocked feeling. You might experience it in one ear or both, and it’s often worse with head colds, allergies, or sinus congestion. The inflammation and mucus associated with upper respiratory infections can prevent the Eustachian tube from opening effectively.
Many people with ETD describe a sensation that their ear desperately needs to pop but won’t. You might hear clicking or popping sounds when you swallow or yawn. Some patients notice temporary improvement when they perform the Valsalva manoeuvre (gently blowing with your nose pinched and mouth closed), only to have the blocked sensation return moments later.
Seasonal allergies, rhinitis, and sinusitis are common contributors to ETD. Anatomical factors also play a role—children have shorter, more horizontal Eustachian tubes, making them particularly susceptible, though adults experience this condition regularly as well.
Most cases of ETD resolve spontaneously as the underlying cold or allergy improves. However, persistent dysfunction lasting more than a few weeks warrants professional assessment. Audiologists can perform tympanometry—a quick, painless test that measures how your eardrum responds to pressure changes—to objectively confirm Eustachian tube dysfunction and monitor improvement over time.
Middle Ear Fluid and Infection
When fluid accumulates in the middle ear space behind your eardrum, it creates a blocked sensation similar to ETD, but the underlying mechanism differs. This condition, known as otitis media with effusion, can occur following upper respiratory infections or as a consequence of prolonged Eustachian tube dysfunction.
The middle ear is normally air-filled. When the Eustachian tube remains blocked, the body absorbs the trapped air, creating negative pressure that draws fluid into the space. This fluid dampens the vibration of your eardrum and the tiny bones (ossicles) that conduct sound, resulting in that characteristic muffled hearing.
Middle ear fluid can persist for weeks or even months, particularly in adults with anatomical predisposition or chronic allergies. Unlike acute ear infections, which cause significant pain and fever, chronic middle ear effusion is often painless but frustrating—your ears feel blocked, but no wax is visible when you (inadvisably) look with a cotton bud.
If pain, fever, or discharge accompany the blocked sensation, you’re likely dealing with acute otitis media—a bacterial or viral infection requiring medical assessment by your GP. This is particularly important in children, though adults certainly develop middle ear infections as well.
Audiologists can identify middle ear fluid through a combination of otoscopy (visual examination of your eardrum) and tympanometry. The characteristic flat tympanogram associated with fluid provides objective confirmation of the diagnosis, helping differentiate it from other causes of blocked ears.
When One Ear Feels Blocked: Considering Asymmetric Causes
If you notice that specifically one ear feels blocked whilst the other remains normal, this asymmetry warrants particular attention. Whilst wax accumulation and Eustachian tube dysfunction certainly occur unilaterally, sudden or persistent blockage in just one ear should prompt consideration of other causes.
Sudden sensorineural hearing loss (SSHL) is an urgent condition where hearing drops significantly—typically in one ear—over a period of hours to days. Many patients initially describe this as a “blocked” sensation before recognising that they’ve actually lost hearing. SSHL may be accompanied by tinnitus (ringing) or vertigo (spinning sensation). This condition requires urgent medical assessment, ideally within 72 hours of onset, as treatment with corticosteroids is time-sensitive and may improve recovery outcomes.
According to Audiology Australia’s clinical practice guidelines, any sudden hearing loss or sudden-onset blocked sensation in one ear that persists beyond 24 hours should be assessed urgently. At The Audiology Place, we maintain emergency appointment availability specifically for these presentations, recognising the time-critical nature of appropriate intervention.
Other causes of unilateral blocked ears include acoustic neuroma (a benign tumour on the hearing nerve), which typically develops gradually over months to years, and Ménière’s disease, characterised by episodic fullness, hearing loss, tinnitus, and vertigo. Temporomandibular joint (TMJ) dysfunction can also create a sensation of ear fullness, typically associated with jaw clicking, facial pain, or recent dental work.
Red Flags: When to Seek Immediate Assessment
Whilst many causes of blocked ears are benign and self-limiting, certain symptoms indicate the need for prompt professional evaluation:
Seek same-day GP or emergency department assessment if you experience:
– Sudden hearing loss in one or both ears (within 72 hours)
– Blocked ear sensation accompanied by severe pain
– Discharge from the ear, particularly if blood-stained
– Blocked sensation following head injury
– Fever alongside ear symptoms
– Sudden dizziness or loss of balance with ear symptoms
– Facial weakness or numbness with ear fullness
Book an audiologist appointment within a few days if you notice:
– Persistent blocked sensation lasting more than two weeks
– Gradual hearing changes that concern you
– One ear feels blocked but no wax is visible
– Your ears feel clogged despite absence of cold or allergy symptoms
– Tinnitus (ringing or buzzing) accompanying the blocked sensation
– History of previous sudden hearing loss
Consider seeing your GP for:
– Blocked ears with fever or significant pain
– Symptoms persisting beyond two weeks despite home management
– Recurrent ear problems requiring investigation of underlying causes
– Blocked ears in the context of broader sinus or allergy concerns
What to Expect During Your Audiology Appointment
When you visit an audiologist concerned about blocked ears, you’ll undergo a systematic assessment designed to identify the specific cause and guide appropriate management.
The appointment typically begins with a detailed case history. Your audiologist will ask about the onset and duration of symptoms, whether one or both ears are affected, associated symptoms like tinnitus or dizziness, recent infections or allergies, and any relevant medical history. This information narrows the differential diagnosis considerably before any testing begins.
Video otoscopy follows—direct visualisation of your ear canal and eardrum using a camera-equipped instrument. This immediately identifies wax accumulation, foreign bodies, eardrum perforation, or obvious signs of infection. At The Audiology Place, we display these images on a screen during the examination, allowing you to see exactly what we’re observing and understand the findings.
If wax isn’t obscuring the view, tympanometry provides objective measurement of middle ear function. This quick, comfortable test involves placing a soft probe in your ear canal that varies air pressure whilst measuring how your eardrum responds. The resulting graph—a tympanogram—reveals whether your middle ear is functioning normally, whether fluid is present, or if Eustachian tube dysfunction exists. The test takes only seconds per ear and provides invaluable diagnostic information.
Comprehensive audiometry (hearing testing) measures your hearing thresholds across frequencies and compares air conduction (sound delivered through earphones) with bone conduction (sound delivered through a headband placed on the bone behind your ear). This comparison helps localise where in your auditory system the problem exists—outer/middle ear versus inner ear/nerve—fundamentally different categories requiring different management approaches.
Based on these findings, your audiologist will either provide treatment (such as wax removal), recommend management strategies (such as decongestants or nasal steroids for ETD), or arrange appropriate referral to your GP or an ear, nose and throat (ENT) specialist if medical or surgical intervention is indicated.
Self-Care Strategies and When They’re Appropriate
For certain causes of blocked ears, careful self-management at home is entirely appropriate as a first step, provided red flag symptoms aren’t present.
If you’re experiencing blocked ears during or immediately following a head cold, supporting Eustachian tube function makes physiological sense. Staying well-hydrated helps thin mucus secretions. Steam inhalation or a hot shower can temporarily ease congestion. Over-the-counter oral decongestants or nasal decongestant sprays (used strictly according to package directions for no more than three consecutive days) may provide relief. Some people find that chewing gum or frequent yawning helps exercise the Eustachian tube and equalise pressure.
For those with seasonal allergies, managing the underlying allergic rhinitis with antihistamines or nasal corticosteroid sprays often resolves associated ear symptoms. However, if symptoms persist beyond two weeks despite these measures, professional assessment is warranted.
What should you avoid? Cotton buds, bobby pins, or any objects inserted into your ear canal risk pushing wax deeper, traumatising the delicate ear canal skin, or even perforating your eardrum. Ear candling—a practice involving placing a lit, hollow candle in the ear—is not supported by evidence and carries significant risks of burns and injury without demonstrated benefit. Home irrigation using syringes purchased online risks ear canal trauma and introduces infection risk if not performed with appropriate technique and sterile solution.
If you’re uncertain about the cause of your blocked ears, or if simple measures don’t provide relief within a reasonable timeframe (generally one to two weeks), professional assessment is both safer and more effective than continued home experimentation.
The Importance of Accurate Diagnosis
The sensation of blocked ears is a symptom, not a diagnosis. Whilst this distinction might seem academic, it has practical importance for your care. Treating presumed wax build-up with oil drops when the actual cause is middle ear fluid wastes time and prolongs your discomfort. Similarly, assuming Eustachian tube dysfunction when sudden sensorineural hearing loss is present can result in missed opportunities for time-critical intervention.
This is where the expertise of audiologists and medical practitioners becomes valuable. Professional assessment with appropriate diagnostic tools—video otoscopy, tympanometry, and audiometry—provides objective information that guides evidence-based management rather than trial-and-error approaches.
Furthermore, persistent or recurrent blocked ears may indicate underlying conditions requiring investigation. Recurrent middle ear effusion in adults, for example, warrants nasopharyngeal examination to exclude rare causes. Progressive unilateral symptoms require different consideration than bilateral, fluctuating complaints.
Moving Forward With Confidence
The sensation of blocked ears, whilst frustrating, is rarely dangerous—but it does merit appropriate attention. Understanding the common causes, recognising red flag symptoms, and knowing when to seek professional help empowers you to make informed decisions about your ear health.
If your ears feel blocked and the sensation persists beyond a few days, doesn’t improve with simple measures, or causes you concern—particularly if one ear feels blocked whilst the other remains normal—booking an assessment with an audiologist or your GP is a sensible next step. Early, accurate diagnosis typically leads to quicker resolution and helps identify the small percentage of cases requiring urgent intervention.
At The Audiology Place, we maintain capacity for same-day or next-day appointments for concerning ear symptoms, recognising that persistent blocked ears significantly impact your quality of life and, in rare cases, may signal time-sensitive conditions. We’re independent practitioners committed to brand-agnostic, evidence-based care that prioritises your hearing health above commercial considerations.
Frequently Asked Questions
**Why do my ears feel blocked but there’s no wax?**
Blocked sensation without visible wax typically indicates a middle ear issue rather than an outer ear canal problem. The most common causes are Eustachian tube dysfunction or middle ear fluid, both of which occur behind your eardrum in the middle ear space. These conditions prevent your eardrum from vibrating normally, creating that characteristic fullness. Tympanometry performed by an audiologist can objectively identify these conditions even though nothing appears abnormal when looking into your ear canal.
**How long should I wait before seeing someone about blocked ears?**
If you’ve recently had a cold or allergies and your ears feel blocked, waiting one to two weeks whilst supporting natural resolution with hydration and possibly decongestants is reasonable—provided you’re not experiencing pain, sudden hearing loss, or other concerning symptoms. However, if one ear suddenly feels blocked (particularly if accompanied by hearing reduction or tinnitus), assessment within 24-72 hours is important to exclude sudden sensorineural hearing loss. When in doubt, earlier assessment provides peace of mind and, in some cases, prevents complications.
**Can blocked ears cause permanent damage?**
Most causes of blocked ears—including wax accumulation, Eustachian tube dysfunction, and even temporary middle ear fluid—resolve completely without permanent effects when appropriately managed. However, certain conditions require timely intervention to optimise outcomes. Sudden sensorineural hearing loss, for example, has a time-sensitive window for corticosteroid treatment. Chronic, untreated middle ear fluid can occasionally lead to eardrum changes or chronic ear disease. This is why persistent symptoms warrant professional assessment rather than indefinite waiting.
**Is it safe to use over-the-counter ear drops for blocked ears?**
Wax-softening drops (typically containing olive oil, almond oil, or carbamide peroxide) are generally safe for short-term use if your eardrum is intact and you’re not experiencing ear pain or discharge. However, they’re only appropriate if wax is actually the cause of your symptoms. Using ear drops when the blockage is due to middle ear fluid or Eustachian tube dysfunction won’t help and may delay appropriate treatment. If drops don’t improve your symptoms within three to five days, discontinue use and seek professional assessment. Never use ear drops if you have a history of eardrum perforation or have ear tubes (grommets) in place without specific medical advice.