An anonymised case study from The Audiology Place
A man in his early forties, living on Sydney’s Northern Beaches, was referred to The Audiology Place by his GP after noticing a sudden change in his right-sided hearing a few months earlier.
He described a sensation that “felt like water in the ear” and, for several days, sounds on that side seemed as if they were coming “from inside a barrel”. While this initial fullness slowly subsided, he was left with a persistent sense that his right ear felt “heavier” and that there was a disconnect between what he could hear and what he could understand, especially when tired or after a long workday.
He also noticed:
- Difficulty following conversation from his right side unless he turns to face the speaker
- Occasional complete blockage of the right ear in the shower, taking time to clear
- Intermittent high-pitched, non-pulsatile tinnitus in the right ear
He had no significant history of ear infections, no ear pain or discharge, no vertigo, no significant noise exposure and no known family history of hearing loss.
Assessment at The Audiology Place
We approach any sudden or one-sided hearing change very seriously. The goals in this case were to:
- Understand the history and pattern of the change
- Rule out common causes such as ear-canal blockage or middle-ear fluid
- Identify whether the problem was in the outer, middle or inner ear (or a combination)
- Decide if urgent medical review was needed
Dr Signe Steers, Clinical and Paediatric Audiologist, carried out a complete 90-minute diagnostic assessment, including:
- Detailed case history
- Microscopic otoscopic examination
- Tympanometry and acoustic reflex testing
- Comprehensive pure tone audiometry (including extended high frequencies)
- Distortion Product Otoacoustic Emissions (DPOAEs)
- Speech discrimination testing
- Speech in Noise testing
What the tests showed
#image_title
- Ear examination and middle ear function
Under the microscope, both ear canals were clear and healthy, with no wax or debris. The eardrums looked normal on both sides.
Standard tympanometry (a measure of eardrum movement and middle ear pressure) showed:
- Normal middle ear pressure and mobility in both ears
- No signs of middle-ear fluid, eustachian tube dysfunction or apparent stiffness of the eardrum
At this point, the ears looked healthy, and the middle ear measured as functioning normally – an important clue that the problem was not as simple as wax or fluid.
- Hearing thresholds (audiogram)
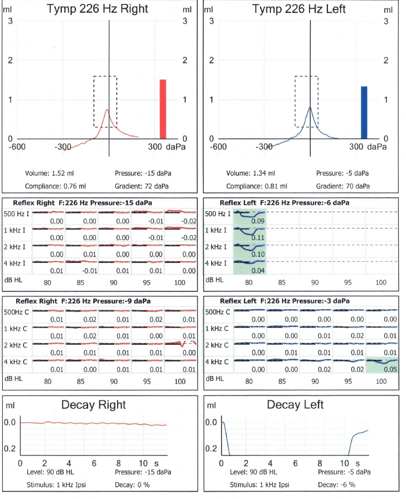
Pure tone audiometry revealed:
- Left ear: Hearing within normal limits across standard frequencies, with only a mild drop in the very high (extended high-frequency) range
- Right ear: A mild to moderate loss in the low frequencies, improving toward the higher frequencies, with evidence of a conductive component (a gap between air- and bone-conduction results) across several frequencies
Interestingly, this conductive overlay in the right ear was not consistent with the normal tympanometry. This pattern can occur in certain middle-ear conditions where the eardrum appears and usually measures, but the tiny bones of hearing (ossicles) are affected.
There was also a slight dip in the bone-conduction scores around 1.5–2 kHz on the right side (often referred to as a Carhart notch), a feature that can be associated with some ossicular conditions such as otosclerosis. Importantly, this is a suspicious pattern, not a diagnosis in itself – that step belongs to an Ear, Nose and Throat (ENT) specialist.
#image_title
- Inner ear function (DPOAEs)
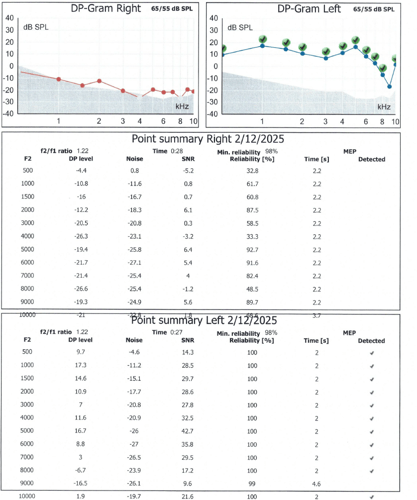
DPOAEs measure the function of the outer hair cells in the cochlea – the sensory cells responsible for amplifying and fine-tuning sound.
- Left ear: DPOAEs were present across the tested frequency range, consistent with normal inner ear function
- Right ear: DPOAEs were absent, suggesting reduced function of the outer hair cells in that ear
This combination – a conductive-looking loss with normal middle-ear pressure, absent otoacoustic emissions, and a Carhart-like notch – raised concern about a more complex underlying issue involving the sound-transmission pathway and possibly the inner ear on the right side.
Next steps: Collaboration with ENT
Given the asymmetry, the patient’s history of a sudden-onset right-sided change, and the atypical pattern on testing, Dr. Steers recommended prompt medical review with an ENT specialist.
A same-week appointment was arranged for further medical assessment and imaging as required. The audiological results and interpretation were forwarded to both the GP and ENT so that all parties had a clear picture of:
- The exact nature and degree of hearing loss in each ear
- The typical appearance and function of the eardrums and the middle ear
- The absent right-sided otoacoustic emissions
- The reasons we were concerned about an underlying middle and/or inner ear pathology, rather than simple wax or fluid
The patient was counselled about the findings in clear, everyday language, including why medical review was essential and which conditions the ENT might consider. He was reassured that he had done the right thing by seeking help rather than ignoring the symptoms once the “blocked” feeling had partially settled.
What this case teaches us
This case highlights several key messages about hearing health:
- A normal-looking ear can still have a significant problem.
You can have a normal-appearing eardrum and normal middle-ear pressure yet still have a conductive-type hearing loss and inner-ear changes. That’s why relying on “it looks fine” isn’t enough. - One-sided changes should never be ignored.
A new or sudden change in hearing in one ear, especially with tinnitus or a sensation of fullness or heaviness, always warrants a thorough assessment and often ENT review. - Advanced testing adds essential pieces to the puzzle.
Extended high-frequency testing and DPOAE measurements, as routinely offered at The Audiology Place, can pick up subtle inner ear changes that might otherwise be missed. - Team-based care matters.
Optimal management of complex hearing changes depends on close collaboration between the GP, audiologist and ENT specialist. Our role at The Audiology Place is to provide precise, evidence-based audiological assessment, clear communication, and ongoing support for the patient and their doctors.
If you notice similar symptoms
If you experience:
- A sudden or recent change in hearing in one ear
- A feeling of heaviness, fullness, or “blocked” sensation that doesn’t resolve
- Difficulty understanding speech on one side, especially in noise or when tired
- New tinnitus in one ear
It is essential to seek a comprehensive hearing assessment rather than waiting to see if it goes away.
At The Audiology Place in Sydney, we take the time to listen to your story, carry out detailed testing, and, when needed, work closely with your GP and ENT to ensure you receive timely, appropriate care.
If you’re concerned about a change in your hearing, you’re very welcome to contact us to discuss whether a complete diagnostic assessment is right for you.